Why does varicose veins occur?
What causes varicose veins in your feet and how to prevent it?
Why does varicose veins occur?
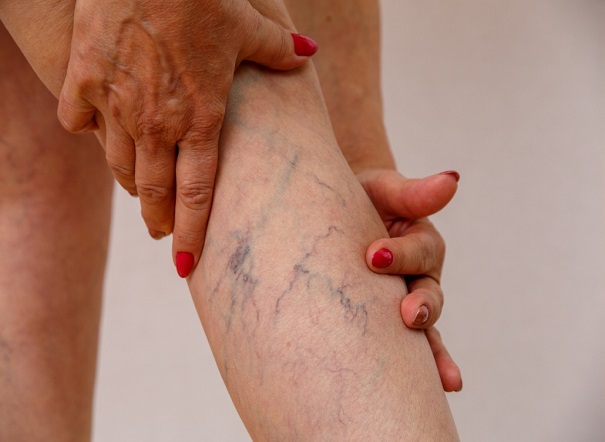
If you are over 40, you will probably see purple blood vessels that have suddenly formed on your leg. Veins are soft, thin-walled vessels that carry blood from your arms and legs to your heart. Because these veins must work against the direction of the earth’s gravitational force, they have valves that only allow blood to pass upward and prevent it from returning back. Your legs and arms have two main types of vessels: superficial and deep vessels. Superficial vessels are close to the surface of the skin and you can often see them. Deep vessels are located near the bones and are surrounded by muscles. The connection of superficial and deep vessels leads to the formation of a third type of vessels called the perforating vein. The contraction of the muscles in the arms and legs during exercise helps to flow through the veins.
Varicose veins are enlarged veins that are felt under the skin and are usually more than 3 mm in diameter. These vessels are usually located in the leg or thigh and cause varicose veins due to weak wall or dysfunction of the vascular valves. These vessels, under the pressure of the earth’s gravitational force, enlarge and after a while rise and twist, and eventually thicken.
How to diagnose varicose veins:
Diagnosis of varicose veins is made by an initial physical examination. The accuracy of the clinical examination is increased with the help of a hand-held Doppler tool in which the doctor can also hear the sound of blood flow. The most accurate and complete test is the Doppler ultrasound test, which shows vascular obstruction due to the presence of blood clots and examines the function of vascular valves. Measurement of venous function in the legs may also be done with other tests, such as plethysmography. This test is not painful.
Factors that increase the risk of varicose veins:
The most important factors that increase the risk of varicose veins are as follow:
- Inheritance
- Common among female
- Lifting heavy things
- Pregnancy, the hormones affect the walls of the veins and makes them more flexible.
- Sedentary lifestyle and high blood pressure are also associated with the formation of varicose veins among women.
- Old age because the elasticity of the vessels decreases with age.
- Obesity and overweight because too much weight increases the pressure on the vessels.
- Damage to the leg’s vessels or blood clots in the superficial or deep vessels in the past
- Prolonged standing for a long time, for example, standing all day
As mentioned, many people with varicose veins have an inherited disease background. On the other hand, the combination of hereditary background with any of the predisposing factors in varicose veins, such as smoking, standing and sitting for a long time and immobility, overweight and obesity, chronic constipation, taking hormonal drugs and many other factors cause varicose veins in the legs. Eliminating the risk factors for varicose veins will lead to definitive treatment for varicose veins in the long period.
Of course, if you developed varicose veins during pregnancy, it is good to know that fortunately, varicose veins usually get better within 3 to 12 months after delivery.
How prevent varicose veins:
You cannot do anything about hereditary factors, age and gender, but you can delay or prevent the progression of varicose veins.
- Be active. Moving your leg muscles will get your blood flowing.
- Keep your blood pressure under control.
- To temporarily relieve symptoms, lie down and place your feet at least 15 cm above the level of your heart. Repeat this several times a day for 10 minutes each time.
- Keep a healthy weight.
- Use varicose socks as directed by your doctor.
- See a specialist who can diagnose the cause of varicose veins and the source of venous reflux in the leg, as well as offer you a variety of treatments.
Varicose veins home treatment:
If the varicose veins do not cause any discomfort, the patient may not want to be treated. Most varicose veins do not cause chronic or long-term problems and do not pose a risk to blood circulation.
The doctor teaches the patient certain activities so that he can relieve his symptoms. Losing weight and engaging in moderate physical activity, such as swimming or walking, is helpful. In addition, you should avoid standing for long periods, as this will aggravate the symptoms. If the patient raises his legs while sleeping, his pain will decrease.